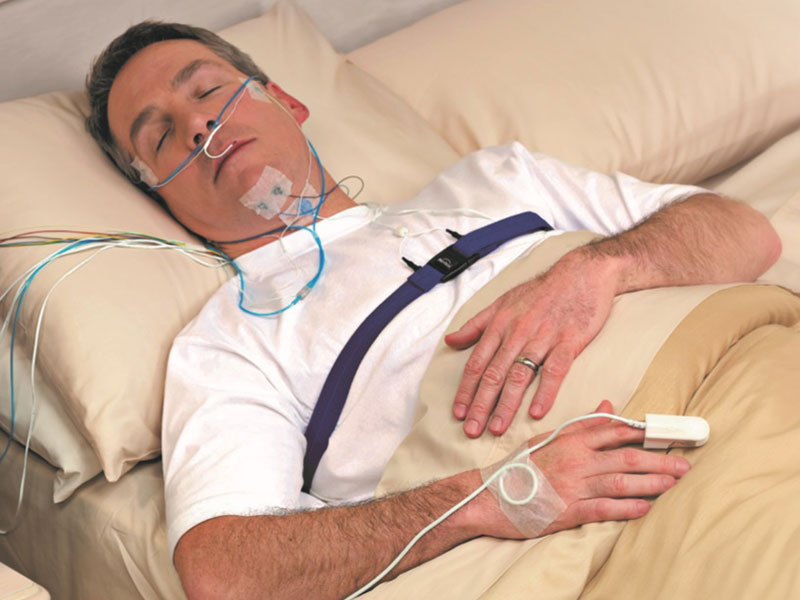
Most people picture one device doing everything, but “sleep study machine” usually means a set of sensors connected to a recorder. Whether it happens in a lab or at home, the goal is the same: capture a clean, minute by minute story of how someone breathes while they sleep.
What is a “sleep study machine” actually measuring?
A sleep study machine measures breathing-related signals rather than “breathing” directly. The core signals are airflow, respiratory effort, and oxygen saturation, plus context signals like heart rate, body position, snoring, and sleep stage in full lab studies.
Those signals let clinicians tell the difference between an obstructed airway, a brain signal problem, or brief normal changes that happen when someone rolls over or enters a new sleep stage.
How does it track airflow through the nose and mouth?
Airflow is usually tracked with a nasal pressure cannula, a soft tube that sits at the nostrils and senses tiny pressure changes as air moves. Many studies also use a thermistor near the nose or mouth to sense temperature shifts between inhaled and exhaled air.
When airflow drops by a certain percentage for long enough, the software flags a hypopnea or apnea candidate. Clinicians then confirm it against the other signals so normal variations are not mislabeled.
How does it know whether the chest is still trying to breathe?
Respiratory effort is measured with two stretchy belts, one around the chest and one around the abdomen. These belts detect expansion and contraction, showing whether the body is attempting to pull air in.
This is crucial for sorting events. If airflow stops but the belts keep moving, it suggests obstructive sleep apnea. If airflow stops and the belts also go quiet, it suggests a central apnea pattern.
How does it track oxygen levels during sleep?
A pulse oximeter, usually on a finger, shines light through the skin to estimate blood oxygen saturation (SpO₂). It also provides a pulse waveform that can hint at motion or poor signal quality.
Drops in SpO₂ that follow reduced airflow strengthen the case that a breathing event is clinically meaningful. Many reports focus on how often oxygen dips occur and how low the saturation falls.
How does it capture snoring and airway vibration?
Snoring can be captured by a small microphone on the throat or chest, or inferred from vibration sensors and airflow turbulence. Some systems also use the nasal pressure signal to detect “flow limitation,” a flattened airflow shape that suggests narrowing.
This helps explain why someone may be working harder to breathe even when oxygen does not drop dramatically. It also supports treatment decisions when symptoms are strong but event counts seem borderline.
How does it tell what sleep stage someone is in?
In a lab polysomnogram, sleep stage comes from EEG (brain waves), EOG (eye movements), and EMG (muscle tone) sensors. These show when someone is awake, in light sleep, deep sleep, or REM.
Staging matters because breathing can worsen in REM or when lying on the back. Without staging, an at home test can still detect many breathing disorders, but it cannot fully explain when and why events cluster.
How do home sleep tests track breathing without all the lab sensors?
Home tests typically focus on airflow, effort, and oximetry, sometimes adding snore and position. They do not usually include EEG, so they estimate “recording time” rather than true sleep time.
That difference can affect event rates because someone may lie awake while the device is still recording. For many people with suspected obstructive sleep apnea, though, the simplified setup captures enough data to make a clear call.
How does the machine decide what counts as an apnea or hypopnea?
Scoring rules use thresholds for how much airflow falls and how long it stays reduced, often paired with oxygen drops or arousal markers. In labs, arousals can be seen in EEG; at home, oxygen and effort patterns carry more weight.

The machine software flags candidates, but trained scorers verify them because leaks, mouth breathing, motion, or sensor shifts can mimic events. The final report usually includes an index, like AHI, showing events per hour. Compare private vs public sleep study cost and options to understand which pathway better suits their needs.
What can distort breathing data overnight?
Loose cannulas, displaced belts, cold fingers affecting oximetry, and frequent movement can all degrade signals. Mouth breathing can reduce nasal pressure readings even when someone is still moving air.
Good systems show signal quality in real time or record markers that help interpreters discount bad segments. If too much of the night is unusable, they may repeat the study to avoid a misleading diagnosis.
What happens to the breathing data after the study ends?
The recorder stores time stamped channels that are uploaded to analysis software. A technologist or clinician reviews airflow, effort, oxygen, heart rate, and related markers across the night.
They then produce a summary: event counts, oxygen statistics, snore patterns, and how breathing changes with position or sleep stage. That final interpretation guides next steps, such as CPAP titration, oral appliance evaluation, or further testing.
FAQs (Frequently Asked Questions)
What does a sleep study machine measure to track breathing during sleep?
A sleep study machine measures breathing-related signals such as airflow, respiratory effort (chest and belly movement), blood oxygen saturation, heart rate, body position, snoring, and sleep stages. These signals help clinicians understand how someone breathes throughout the night and identify any abnormalities.
How is airflow through the nose and mouth monitored in a sleep study?
Airflow is typically tracked using a nasal pressure cannula, which senses tiny pressure changes at the nostrils as air moves. Additionally, a thermistor near the nose or mouth detects temperature shifts between inhaled and exhaled air. When airflow drops significantly for a certain duration, it may indicate hypopnea or apnea events.
How does the sleep study machine determine if the chest is still making breathing efforts?
Respiratory effort is measured using two stretchy belts placed around the chest and abdomen. These belts detect expansion and contraction movements showing whether the body is attempting to breathe. This helps differentiate between obstructive sleep apnea (effort continues despite airflow stopping) and central apnea (both effort and airflow stop).
What role does oxygen saturation monitoring play in a sleep study?
Oxygen levels are tracked using a pulse oximeter, usually attached to a finger, which estimates blood oxygen saturation (SpO₂) by shining light through the skin. Drops in SpO₂ following reduced airflow indicate clinically significant breathing events. Oxygen data supports diagnosis and helps assess severity of breathing disorders during sleep.
How are snoring and airway vibrations detected during a sleep study?
Snoring can be recorded by a small microphone placed on the throat or chest or inferred from vibration sensors and airflow turbulence patterns. Some systems also analyze nasal pressure signals to detect flow limitation – a flattened airflow shape suggesting airway narrowing. This information helps explain increased breathing effort even when oxygen levels remain stable.
How do home sleep tests differ from lab studies in tracking breathing during sleep?
Home sleep tests generally focus on measuring airflow, respiratory effort, and oxygen saturation, sometimes adding snore detection and body position sensors. Unlike lab polysomnography, they typically do not include EEG to determine exact sleep stages, so they estimate recording time rather than true sleep time. Despite this simplification, home tests often provide sufficient data to diagnose obstructive sleep apnea effectively.

